What are scars?
Introduction
Scars form as a natural part of the body’s healing process after skin damage. When the skin sustains an injury, it repairs itself by generating new tissue to close the wound and fill in any gaps created by the injury. This tissue, known as scar tissue, is primarily composed of collagen. The appearance of a scar depends on various factors such as the type of injury, the location of the wound, treatment methods, and even genetic factors.
What is Scar Tissue?
Scar tissue is a collection of cells and collagen that covers the site of an injury. Unlike normal skin, scar tissue has distinctive characteristics due to its unique structural makeup
Factors Influencing Scar Appearance
Several factors affect how a scar looks, including:
- Cause of injury: Such as surgery, burns, or severe acne
- Wound size, severity, and location
- Treatment: Whether the wound received stitches or bandages
- Individual differences: Age, genetics, ethnicity, and overall health
Characteristics of Scar Tissue
Scar tissue exhibits certain characteristics that differentiate it from normal skin:
- Disturbed alignment of collagen fibers
- Excessive dermal fibrosis
- Absence of elastic fibers and skin appendages
- Altered skin texture
Types of Scar Tissue
- Mature Scars: These can be categorized into normal, atrophic (depressed), or hypertrophic (raised).
- Contracture Scars: Typically caused by burns, contracture scars tighten the skin, limiting movement, especially when involving muscles, nerves, or joints.
- Depressed (Atrophic) Scars: Sunken scars commonly result from chickenpox or acne and are often referred to as “ice pick scars.”
- Flat Scars: These scars appear pink or red initially, eventually becoming lighter or darker than the surrounding skin.
- Keloids: Raised scars that extend beyond the initial wound area; these can become quite large and may restrict movement.
- Raised (Hypertrophic) Scars: Elevated scars that stay within the wound boundary but never completely flatten.
- Stretch Marks: Form when the skin rapidly expands or contracts, damaging connective tissue beneath, often occurring during pregnancy, puberty, or significant weight changes.
Clinical Differences Between Keloids and Hypertrophic Scars
- Keloids: Non-severe, commonly found on the chest, upper back, or earlobe. Symptoms include erythema, itching, and pain, and they spread beyond the wound area.
- Hypertrophic Scars: Often due to burns or incisions, these can occur anywhere on the body and present symptoms like erythema and itching but remain within the wound area.
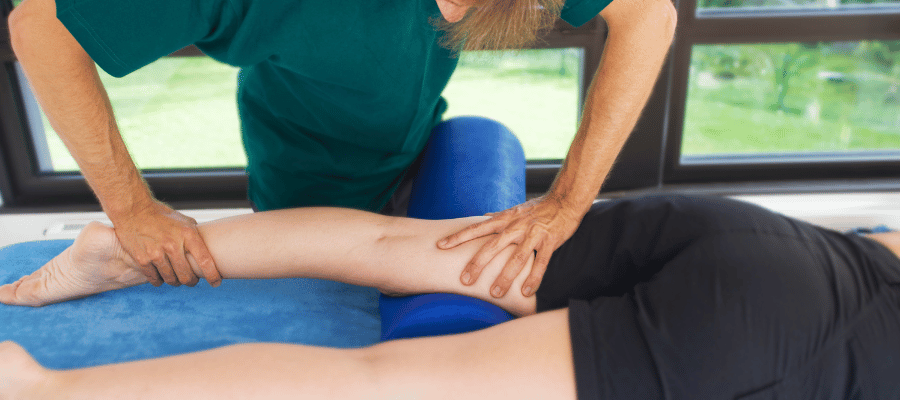
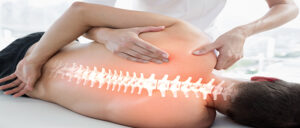
Physiotherapy Treatment for Scars
Physiotherapy offers effective methods to prevent scar adhesions, reduce discomfort, and improve tissue functionality. Techniques include:
- Lymphatic Drainage and Scar Mobilization: Reduces adhesions, improves skin pliability, and reduces scar thickness.
- Kinesiotaping: Helps relax fascia, improve nourishment, reduce edema, and prevent excessive tissue growth.
- Dry Needling: Effective for decreasing pain and improving scar mobility. In older scars, dry needling stimulates collagen formation and skin regeneration.
- Instrument-Assisted Soft Tissue Mobilization (IASTM): Removes scar tissue and promotes functional normalization of soft tissue by reinitiating the healing process and increasing blood flow.
Conclusion
Scar tissue formation is an essential part of the healing process, but it can often lead to pain, restricted movement, and aesthetic concerns. Physiotherapy plays a significant role in managing scar tissue by improving tissue flexibility, reducing scar thickness, and restoring function. Using techniques like scar mobilization, dry needling, and IASTM, physiotherapy can provide comprehensive care and rehabilitation for individuals dealing with scar tissue complications.