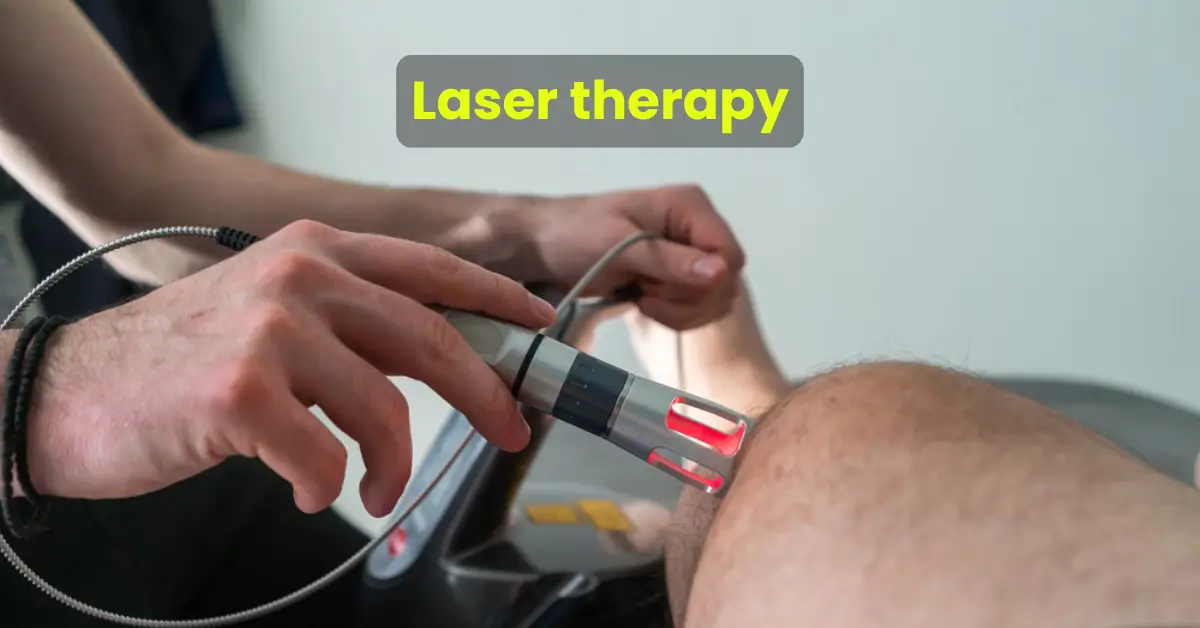
Laser therapy
INTRODUCTION
LASER is an acronym for light amplification by stimulated emission of radiation. Radiation is the process by which energy is propagated through space. The common characteristics of all forms of radiant energy are.
- They are produced by applying electrical or other forces to various forms of matter .
- They all may be transmitted without the support of a sensible medium.
- Their velocity of travel is equal in a vacuum but may vary within different media.
A laser is generally used as a source or generator of radiation. The low power laser is used in physical rehabilitation for pain control and soft tissue injury.
Bio-stimulating, regenerating and pain killing in its effect, laser treatment opens up an extraordinarily large indication spectrum, and it has uncomplicated, completely painless, fascinating and pleasant effect upon patients and is used in the following:
- Orthopaedics, traumatology, rheumatology (treatment of inflammatory or degenerative rheumatic disease, post-traumatic conditions, bones Pathologies, oedemas, haematomas).
- Neurology (neuralgias, migraines, neuritis).
- Dermatology (treatment of chronic ulcers, burns, herpes infections, rhagades).
- Surgery (post-operative complications, regen- eration of ruptured or severed nerves and tissues).
- Odontology (complex treatment stomatitis, aphthae, herpes infections, gingivitis, treatment of the pulp, alveolitis, pathology of the temporomandibular joint).
- ENT (treatment of acute and chronic otitis, sinusitis).
- Gynaecology (inflammatory diseases of the pelvic region, post-operative complications, conditions. After abortions).
DOSAGES
Actual dosage with the cold laser depends on the power factor, duration of radiation, and tissue resonance. Focusing the beam properly will bring into play the inverse square and cosine laws, so that distance-to-target and angulation of beam-to-target will affect the dosage administered.
PAIN CONTROL
At acupuncture trigger points, nerve roots and pain sites, a dosage of 15 to 30 seconds for each point is recommended. Unlike for the open wounds, the probe tip is held in contact with the skin at these points during the procedure.
MODES
Current laser equipment offers the clinician two modes -continuous and pulsed beams.
- Continuous Beam: The continuous mode is recommended for acute pain and fresh wounds.
- Pulsed Beam: The pulsed mode has been found more effective with chronic conditions. Pulsed models vary from 1 to 80 pulses per second, depending on the manufacturer. One suggested technique for chronic pain or long-standing open lesions would be in the range of 4 to 10 pulses per second.
INDICATIONS
1. Wound healing-The photo-biostimulation of wound healing remains the cardinal indication for therapeutic laser in physiotherapy. In this, laser therapy has come to be recognized by many therapists as superior to a range of other alternative electrotherapeutic modalities including ultrasound .In case of scarring, it has been reported by some therapists that laser therapy may not only accelerate remodelling of the scar tissue but also give a more cosmetically acceptable result.
In soft tissue injuries – traumatic, inflammatory and overuse type injuries. While variable results have been reported for the laser treatment of bursitis and muscle spasm, other common soft tissue injuries such as muscle tears, haematomas and tendinopathies would seem to respond particularly well to therapeutic laser, which has led to its wide use in sport medicine.
For pain relief – including both acute pain (e.g., post- operative pain) and more chronic pain syndromes such as herpes zoster/post-herpetic neuralgia, laser application is common but for the lack of an obvious mechanism of action and the conficting findings of clinically based research.
In arthritic condition – various aetiologies, particularly where these have affected the small joints of the hands and/or feet.
- Reduction of the oedema and hyperaemia
- Promotion of the wound healing .
CONTRA-INDICATIONS
- Do not radiate the eye directly.
- Whether pregnancy is a contra-indication to use of the laser has not yet been determined, but the laser is suspected due to its mobilizing effect on steroids in the human system.
Do not use laser with patients who are naturally photosensitive or who are photosensitized by the medications.
PRECAUTIONS
Poor results may ensue in those patients:
- Extreme age
- Under heavy medication
- With thick eschar
- With considerable scar tissue
- With extremely dry skin
- With active infection.
“At Arunalaya Healthcare, we pride ourselves on being the best physiotherapy center in Delhi. Our dedicated team of experts offers top-notch physiotherapy treatment tailored to your needs. Experience the difference with the leading physiotherapy clinic in Delhi area. Our commitment to excellence ensures that you receive the best physiotherapy care possible. Trust Arunalaya Healthcare for the best physiotherapy treatment in Delhi. Our advanced physiotherapy solutions set us apart as the premier choice for your rehabilitation needs. When it comes to physiotherapy, our center stands out as the best in Delhi. Choose Arunalaya Healthcare for comprehensive physiotherapy solutions that deliver results. Visit Arunalaya Healthcare today and discover why we are the best physiotherapy center in Delhi.”